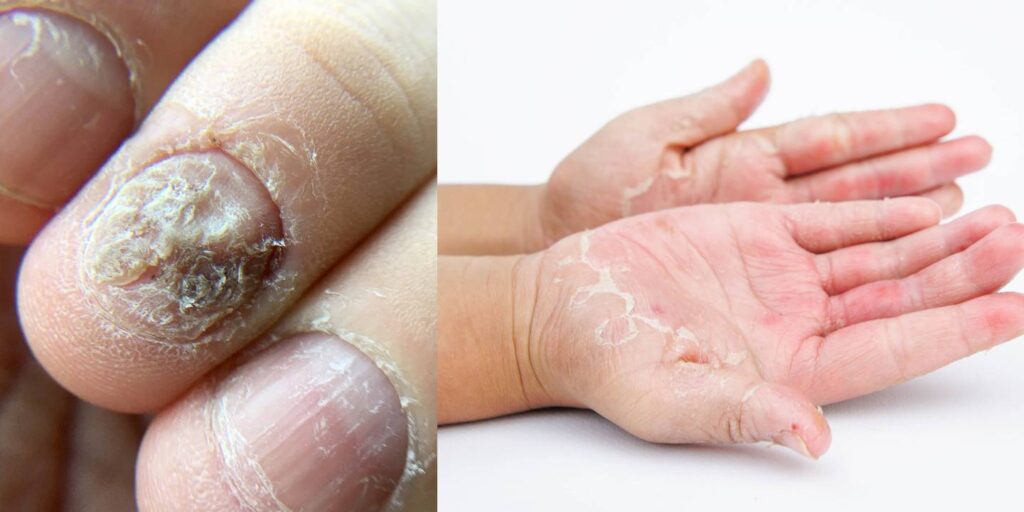
Psoriasis and fungal infections are common skin conditions that have symptoms very similar to each other, making it challenging to distinguish between them. If you are sitting there wondering what these symptoms you are experiencing, be assured that you aren’t alone.
While psoriasis is an autoimmune disorder that results in the rapid growth of skin cells, leading to the formation of thick, scaly patches, fungal infections are caused by various types of fungi and can manifest as red, itchy, and sometimes scaly patches on the skin.
Since the symptoms of these two skin disorders are similar, distinguishing between the two can be challenging. This article will explore whether you are suffering from psoriasis or fungal infection and how to distinguish the two.
What are the Clinical presentations of Psoriasis?
To better understand the difference between psoriasis and fungal infection, we first need to pay close attention to the individual conditions, their explanations, and the kind of symptoms that are unique to each of them.
In this case, we are starting with psoriasis.
Psoriasis is a chronic autoimmune condition that affects the skin, causing various symptoms. To this day, the exact cause or trigger behind psoriasis isn’t known, but research indicates that it could be an interplay between genetic and environmental factors.
The following are the primary symptoms of psoriasis:
Red, Raised Patches – One of the hallmark characteristics of psoriasis is the presence of well-defined, raised, and reddish patches of skin. These patches are often covered with a silvery-white scale, resembling plaques.
Silvery Scales – When it comes to psoriasis, the red patches are standard, and these red patches are often covered in silvery scales. The scales develop a few days after the initial breakout and are typically composed of dead skin cells on the site of the flare-up.
Itching and Pain – Psoriasis is not a fun experience since the condition typically leads to chronic itching and pain, depending on the severity of the breakout and the flare-up’s location.
Koebner Phenomenon – In psoriasis, new patches can develop at skin trauma or injury sites. This is known as the Koebner phenomenon and is a characteristic feature of the condition.
Nail Involvement – Not just the skin, some psoriatic patients struggle with the condition affecting their nails, causing discoloration, pitting, and even separation of the nail from the nail bed.
| Related Blogs: Best Psoriasis Treatment in India |
What are the Clinical Presentations of Fungal Infection?
Now that you have an overview of how psoriasis looks and manifests in patients, let us take a look at the symptoms of fungal infections.
Fungal infections are caused by different species of fungi, such as dermatophytes, Candida, and Malassezia. The clinical presentation of fungal infections can vary based on the type of fungus involved.
A few of the most common symptoms include
Red, Scaly Patches – This is one of the most common symptoms, which also coincides with the symptoms of psoriasis. The patches can appear red and inflamed, be of varying shapes and sizes, and lead to itching and discomfort in the patient.
Circular or Ring-like Rash – In some cases, like with ringworm infection, the site of the infection can appear as a ring-like rash on the skin, which makes the diagnosis relatively straightforward for the patient.
Cracking or Peeling Skin – When left untreated, the fungal infections can also cause the skin to crack and peel. It is often very painful and particularly common if the infection is between the toes or groin region.
Nail Involvement – Like in the case of psoriasis, fungal infections can affect the nails, too, leading to discoloration and falling out.
These skin disorders have a set of similar symptoms and a few unique symptoms that are critical to making the correct diagnosis for a tailored and effective treatment plan.
| Related Blog: 9 Best Home Remedies for Psoriasis |
Free Consultation Most Affordable Treatment 1,00,000 + Happy Patients Treatment at Home 25 + years of doctors experience Free Consultation Most Affordable Treatment 1,00,000 + Happy Patients FSSAI Approved Treatment at Home 25 + years of doctors experiencePsoriasis treatment with Kayakalp Global




Approved

Psoriasis treatment with Kayakalp Global






What are the Causes of Psoriasis and Fungal Infections?
Simply reading about psoriasis and fungal infection isn’t enough if you aren’t aware of the causes. It’s essential to explore the underlying scientific reasoning for these conditions to understand the differences between psoriasis and fungal infections.
Psoriasis
Some of the most common causes that contribute to the onset of psoriasis include:
- In psoriasis, there is an immune dysregulation where T cells, a type of white blood cell, play a crucial role. Activated T cells release cytokines, leading to the inflammation and proliferation that cause the build-up of the cells and the redness on the skin.
- The rapid proliferation of keratinocytes is a hallmark of psoriasis, typically caused by the abnormal activation of keratinocytes in response to proinflammatory signals from immune cells.
- Lastly, psoriasis is passed down through generations due to the genetic makeup. Specific genes, such as HLA-Cw6, are associated with an increased risk of developing the condition. If you are genetically predisposed to developing this condition, external factors like infections and trauma can trigger or exacerbate the condition.
| Related Blogs: Top Lifestyle Changes for Psoriasis |
Fungal infections
Some of the common causes that contribute to the onset of fungal infections include:
Fungal infections are caused by various fungi. The type of fungi determines the kind of fungal infection one is suffering from.
- Dermatophytes are the fungi that typically contribute to the onset of infections like ringworm and athlete’s foot by infecting the skin’s keratin.
- The most common types of yeast infections you can think of or have suffered by are caused by Candida species and occur in areas when there is a disruption in the normal skin barrier or changes in the local microenvironment.
- If you are diagnosed with a condition called seborrheic dermatitis, it is a type of yeast infection that’s caused by Malassezia.
Determining these underlying causes can help with an early and proper diagnosis of the patient to ensure they receive the treatment they need to overcome the complications.
| Related Blogs: Yoga Asanas For Psoriasis Treatment |
How are Psoriasis and Fungal Infections Diagnosed?
Various diagnostic approaches can be utilized to differentiate between psoriasis and fungal infections accurately. These may include clinical examination, microscopy, and laboratory tests.
The diagnosis can also determine the difference between fungal infection and psoriasis to ensure the patient gets tailored treatment addressing their rightful concerns.
Clinical examination
This is where our specialists at Kayakalp Global assess the patient’s physical symptoms to determine whether the patient is suffering from a psoriatic flare-up or a fungal infection.
Microscopy
Microscopic examination of skin scrapings or nail clippings can be valuable in diagnosing fungal infections. Determining the type is crucial to prescribing a relevant treatment plan if the patient suffers from a fungal infection.
For this diagnostic process, a sample is collected from the affected area and then studied under the microscope to identify the causative organism.
Laboratory tests
In some cases, laboratory tests may be necessary, mainly when the diagnosis is unclear or when nail involvement is suspected. These tests can include fungal cultures and polymerase chain reaction (PCR) assays to identify the specific fungal species responsible for the infection.
| Related Blog: Do’s and Don’ts in Psoriasis Treatment |
What are the treatment approaches for Psoriasis and Fungal Infections?
Differentiating between psoriasis vs fungal infection is critical because the treatment approaches for these conditions are distinct.
Following is a breakdown of the same one by one.
Treatment for Psoriasis
The treatment of psoriasis aims to reduce inflammation, slow down keratinocyte proliferation, and alleviate symptoms. This is done via:
- Topical Corticosteroids
- Topical Calcineurin Inhibitors
- Topical Retinoids
- Phototherapy
Treatment for Fungal infection
Treatment for fungal infections focuses on eradicating the causative fungus. The choice of treatment depends on the type and location of the infection. This is done via:
- Topical Antifungals
- Oral Antifungals
- Hygiene and Lifestyle Modifications
- Antifungal Shampoos
- Nail removal
Since the treatment approaches for fungal infection vs psoriasis are so drastically different, getting a tailored diagnosis is key. This is why our specialists at Kayakalp Global advise our patients to schedule an early consultation before the symptoms worsen and cause pain and discomfort.
| Related Blog: 11 Best Home Remedies for Scalp Psoriasis Treatment |
Conclusion
Distinguishing between psoriasis and fungal infections can be challenging due to the overlapping clinical features of these conditions. If you are experiencing symptoms like red, inflamed, and itching skin and are confused about whether it’s psoriasis or a fungal infection, getting a professional’s opinion is key.
Accurate diagnosis and appropriate treatment are essential to relieve individuals suffering from these skin conditions. Therefore, a collaborative effort between patients and our specialists at Kayakalp Global can ensure the right course of action and improved quality of life.
| Related Blog: Psoriasis Vs Eczema: What are the difference in symptoms and treatment |
Frequently Asked Questions
Is it possible to have both psoriasis and a fungal infection simultaneously?
Yes, patients can experience both psoriasis and fungal infections simultaneously. In some cases, patients might develop fungal infections after, at the site of their psoriatic flare-ups.
Can psoriasis be triggered or worsened by stress?
Stress is a key trigger behind the flare-ups of psoriasis. It can lead to increased inflammation and exacerbate the patient’s symptoms.
What are the common risk factors for fungal skin infections?
Some common risk factors behind fungal skin infections include excessive moisture or sweating, compromised skin integrity (cuts, scrapes), sharing personal items like towels or combs, and close contact with infected individuals.